Framework for Suicide Prevention: Overview and Evidence Summary
Every problem becomes more manageable when you have a framework.
A Unifying Framework to Guide Suicide Prevention Best Practice Across Roles
The SafeSide Framework is a map of evidence-based and best practices in suicide prevention. The framework is versatile and strategic, having potential for impact at many levels of an organization.
- Individual staff members use the framework to guide, conceptualize, and provide consumers the best the field has to offer.
- Supervisors and teams use the framework as a structure for efficient reviews, co-reflection, and problem-solving.
- Systems and quality improvement leaders use the framework to evaluate and plan improvements to policy, services, and pathways.
- Learning and staff development leaders use the framework and associated resources to identify and address focus areas for suicide prevention education.
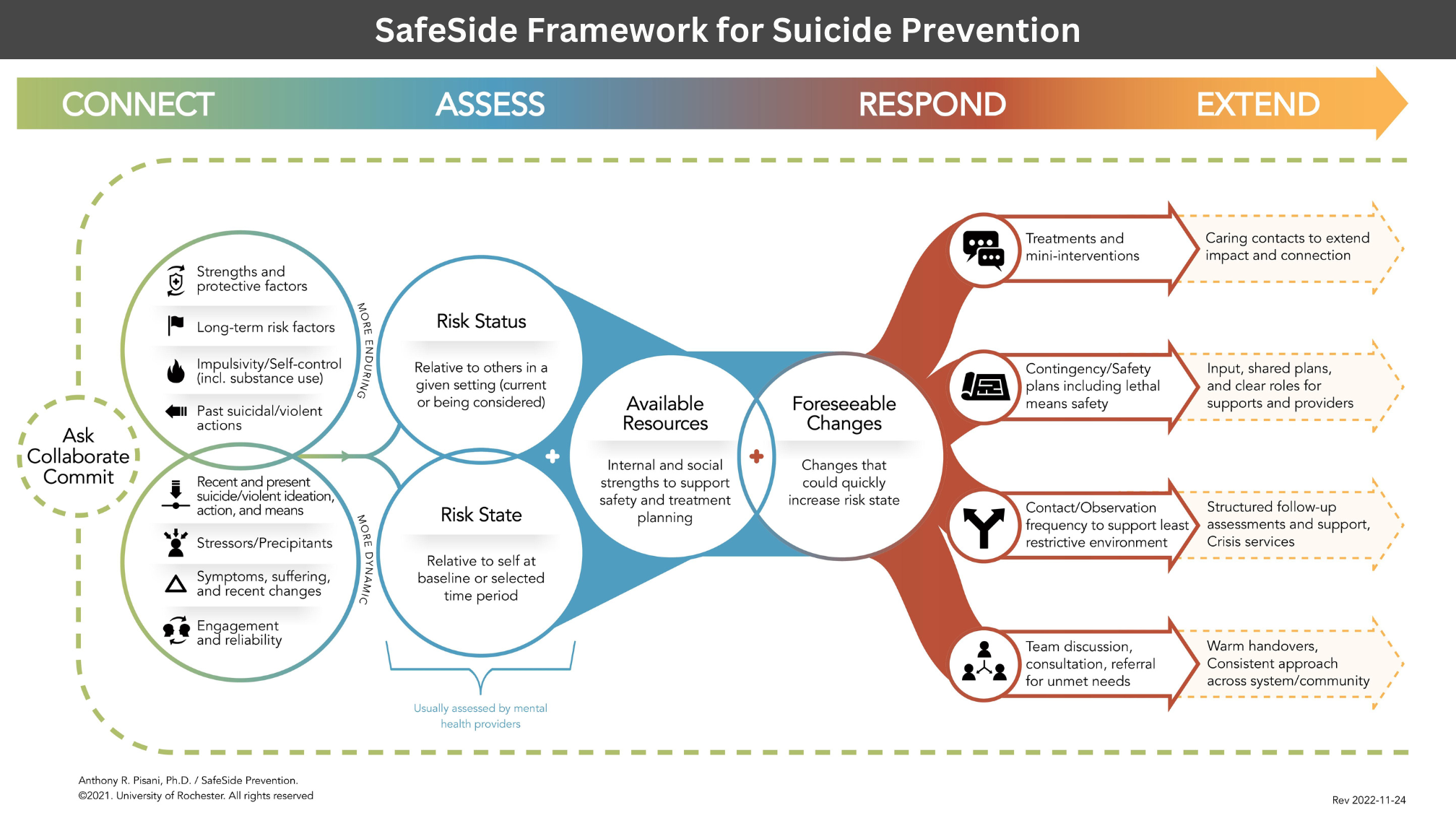
Connect, the foundation, includes asking a person directly about suicide while understanding their individual context (Berman & Silverman, 2017; O'Reilly et al., 2016; Richards et al., 2019a, 2019b), collaborating with the person and their support network, and committing to their safety and well-being over time (Tyndal et al., 2022; Whitlock et al., 2014).
Assess uses a structured approach to gather, organize, and share information to better understand the person. This information is then used to articulate a prevention-oriented risk formulation (Pisani et al., 2022; Pisani et al., 2016) that moves the team towards person-specific plans and supports (Wyder et al., 2021; Turner et al., 2021). Prevention-oriented risk formulation is an important pillar of the Suicide Prevention Pathway implemented by Gold Coast Health in Queensland, Australia (Turner et al., 2020), on which Dr. Pisani advised. Recent evidence from Gold Coast shows a 35% reduction in repeated suicide attempts for those who received care on this Pathway (Stapelberg et al., 2020).
Respond refers to the range of strategies and responses that target suicidal drivers, including evidence-based treatments (Jobes, 2023; Linehan et al., 2015), mini-interventions (Moutier et al., 2021), contingency and safety planning (Knapp, 2023; Pisani et al., 2016, 2022; Nuij et al., 2021; Stanley et al., 2018), means safety (Marcus et al., 2025; Hawton et al., 2024), appropriate observation (Brodsky et al., 2018), and referrals for unmet needs (Renaud et al., 2014).
Extend provides skills that support a person in their life, not just in treatment: non-demand caring contacts (Landes et al., 2021; Reger et al., 2017); collaborative shared plans with clear roles for family, carers, and other supports (Asarnow et al., 2017; Nakao et al., 2008), structured follow-up assessments and support (Mann et al., 2021) and crisis services (Chung et al., 2019; Gould et al., 2022), warm handovers and a consistent approach across systems/communities (Pisani & Boudreau, 2023; Turner et al., 2021).
